  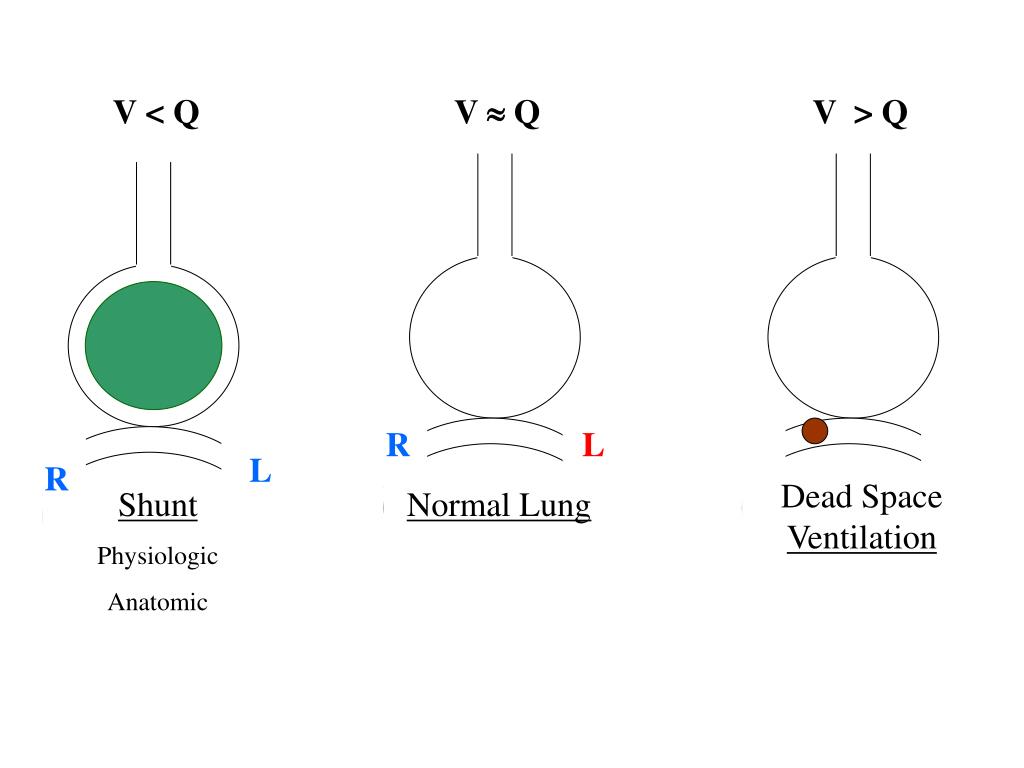
The word gradient is a misnomer, and ideally, it should be referred to as A-a oxygen difference as the difference between alveolar and arterial oxygen is not due to any diffusion gradient. Therefore, hypoxemia due to V/Q mismatch, diffusion limitation, and shunt will have widened gradient, whereas hypoxemia due to hypoventilation would have normal gradient. 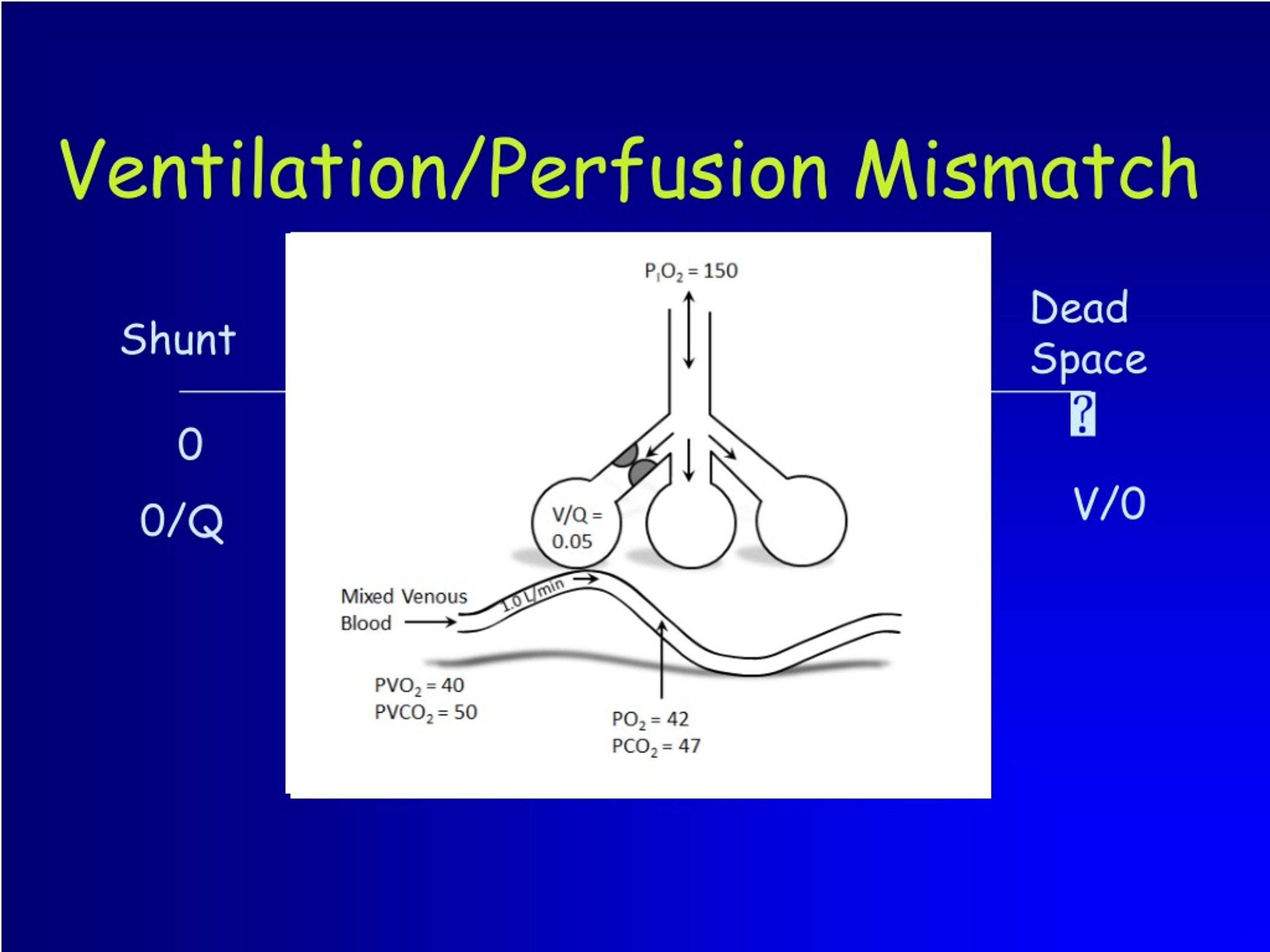
Pathology of the alveolocapillary unit widens the gradient. The A-a oxygen gradient indicates the integrity of the alveolocapillary membrane and effectiveness of gas exchange. Uworld says this is v/q mismatch but that gets me confused cause why wouldn't a vent defect give v/q mismatch.It is the difference between alveolar oxygen level (PAO 2) and arterial oxygen level (PaO 2) and is represented by the following equation: Alveolar to arterial (A-a) oxygen gradient = PAO 2 – PaO 2. That's why you will see a drop in PaO2 in PE(minor). So this one is tougher but: Let's assume you have a well ventilated alveoli, when there is poor oxygen content, vasculature will constrict and redistribute this blood to other alveolar however it will overwhelm the capacity of extracting oxygen into blood - so adding oxygen will help. Dead space/physiologic dead space/V/Q mismatch to inifinty.I remember total pulm shunt as if pulm art partial pressure = pulm vein partial pressure, shunted, basically just bypassed lungs. These alveolar are already extracting maximum oxygen, adding more would not help. Lets assume this kid have some alveoli that are working. pulm shunting - ventilation defect V/Q 0, perfusion intact.So this is my understanding of the topic and I might be wrong so please correct me if thats the case: 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
